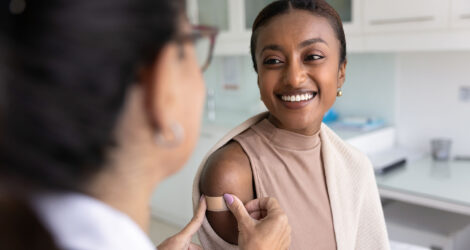
Engagys Medicare Expertise and Experience

Relying on millions of Medicare insights to optimize program results
What works to motivate younger populations to take action on their health isn’t always going to motivate a Medicare population. Conversely, what worked in the past to motivate older members has changed rapidly the last few years as more Medicare members have gotten more comfortable with technology. It’s imperative to draw on Medicare insights when creating programs for this segment. Medicare members are actively involved in their health plan selection and are the group most apt to look for new insurance if they are unsatisfied. Engagys has the expertise and experience to help you optimize the results of your Medicare programs to boost satisfaction, star ratings, and ultimately enrollment.
Engagys Medicare Expertise
Collectively, Engagys consultants have over six decades of experience working with Medicare populations and have reached tens of millions of Medicare members throughout various programs. We draw on insights from past interactions to inform the next project and use test and learn methodologies to improve outcomes. Our consultants have worked and continue to work with large national health plans, health technology companies, providers, nonprofits and many others in the Medicare space.
Engagys Medicare Experience
Engagys supports Medicare health plans in many ways. Below are just a few examples of client programs:
- Optimized Medicare communications across a large national plan by adding behavioral science principles to all outreach to increase results including closing gaps, motivating taking vaccines, and more.
- Transformed CAHPS outreach with a variety of initiatives focused on improving member experience.
- Optimized the enrollment process and technology infrastructure for multiple condition management programs for a Medicare population increasing enrollment rate performance by more than 50%.
- Facilitated healthcare organizations to leverage data from segmentation, targeting, predictive modeling, analytics, and technology to create a positive optimized engagement experience.
Medicare Program Experience
|
|
Tactics to Improve Medicare Program Outcomes
At Engagys, our Medicare solutions are designed with the end consumer in mind. We aim to find the best ways to improve your interactions with members, on an enterprise-by-enterprise basis—customized by client to address specific strengths, weaknesses, and areas of opportunity. For example:
Personalization
Personalization has been proven to increase member engagement in many domains including screenings, medication adherence, and retention.
Results: A personalized pharmacy outreach nearly doubled refill rates over the control.

Barrier Breaking
When sending reminders for preventive care, soliciting why a member is unlikely to make or keep an appointment will increase engagement rates.
Results: Frequent barriers uncovered include lack of transportation, cost, fear of the test or preparation, and simply a belief that the procedure is unnecessary.

Behavioral Economics
Behavioral economics are the messaging tactics that nudge consumers to act.
Results: Applying the Fear of Missing Out (FOMO) tactic with a simple question, “Are you sure,” has been shown to increase healthcare engagement 10% - 30%.

Health Literacy
Many seniors have difficulty comprehending healthcare information. Our work has shown that more frequent communications containing simpler messages will out-perform fewer, more complex messages.
Results: For senior populations, multi-channel outreach confirms that more frequent communications containing simpler messages drive better outcomes than fewer communications with more complex messages.

Communications Governance
Mapping communications inventory to member segments enables an intentional and optimized experience.
Results: A health plan found that a single member received dozens of communications in a single month. Consumers experience communications fatigue when communications are disjointed, too frequent, or not relevant to the member.
Results: Prioritizing, combining, and sequencing can improve engagement rates by 10% or more.

Technology Use
Preference Capture — learn how individual members wish to interact and in which situations.
Results: Adding email as a channel for Medicare members substantially increased compliance with preventive screenings.
SMS text messaging — leverage this channel for personalized communications.
Results: A campaign which added two-way SMS text to an automated hypertension management program nearly doubled the number of members that successfully completed the 12-week program.
Collectively, Engagys associates have over six decades of experience with Medicare populations and insights gained from tens of millions of Medicare member interactions.